This is a comprehensive guide to benzodiazepine addiction treatment that includes key facts about benzodiazepine use, risk factors for substance use disorder, signs to watch out for, benzodiazepine detox and withdrawal symptoms, how to address benzodiazepine use disorder, and the next steps to take with treatment.
What are Benzodiazepines?
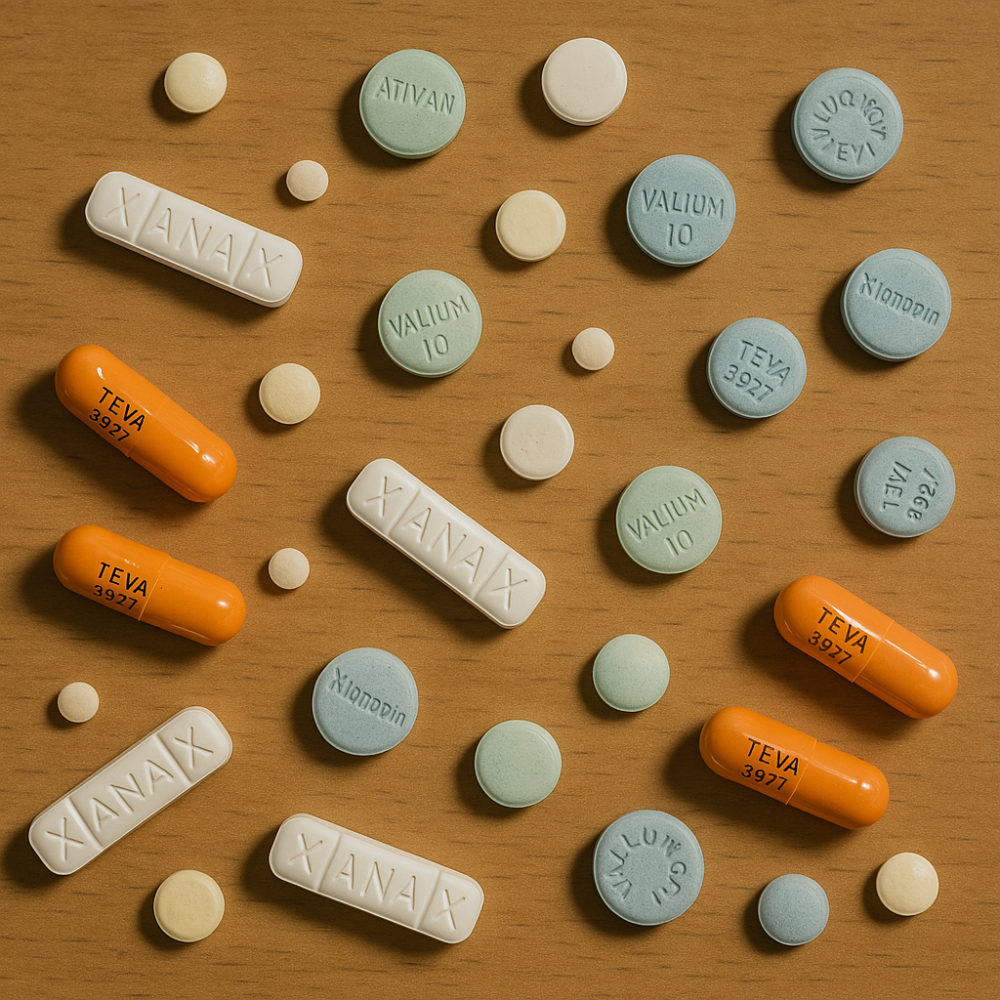
Benzodiazepines (sometimes called “benzos”) are prescription tranquilizers and sedatives that are used to treat anxiety and sleep disorders. They work to calm or help a person sleep by raising the level of neurotransmitter GABA in the brain. Common benzos include diazepam (Valium), alprazolam (Xanax), clonazepam (Klonopin), temazepam (Restoril), and triazolam (Halcion).
Facts and Statistics About Benzodiazepine Use
While benzodiazepines can be effective at managing anxiety and insomnia, taking it for reasons other than what it was prescribed for increases the risk of addiction — a risk associated with taking any benzodiazepine.
Benzodiazepine use as a whole is a serious problem in the United States. According to the National Institute on Drug Abuse (NIDA), more than 30 percent of opioid-related drug overdoses also involve benzodiazepines. NIDA reported that between 1996 and 2013, the number of adults filling a benzodiazepine prescription increased 67 percent, from 8.1 million to 13.5 million.
The American Psychiatric Association (APA) stated that benzodiazepines use is highest among 50-64 year olds. Men are more likely to misuse benzodiazepines than women.
Causes and Risk Factors
The effects of long-term benzodiazepine use include depression, disinhibition, impaired memory and cognitive skills such as response times and coordination, brain damage, and increased risk of car crashes and even hip fractures. They are also prone to misuse.
Stanford psychiatrist Anna Lembke says that physicians “tend to overestimate the benefits” of benzodiazepines. “Long-term use can make insomnia, mood, and anxiety worse.” Those who take benzodiazepines regularly and for a prolonged period of time, risk “dependence, addiction, cognitive damage, more falls, and death,” Lembke contends.
The FDA also warns of the increased adverse effects of using benzodiazepines with medication-assisted treatment drugs (such as buprenorphine and methadone), but concluded that the benefits of treating opioid addiction outweigh the increased risks of drug interactions.
Symptoms and Diagnosis of Addiction to Benzos
Continued use of benzodiazepines can lead to increased tolerance and dependence, causing the person to take more than is clinically indicated in order to feel the euphoric effects. Despite the negative consequences on work, home, and relationships, individuals will still continue to favor the drug. Once dependence occurs, patients will experience side effects, some of which are severe and even life-threatening.
Side effects of increased and prolonged use could include:
- Constipation
- Nausea
- Drowsiness
- Headache
- Dizziness
- Stomach pain
- Restlessness or excitement
- Changes in appetite
- Difficulty urinating or frequent urination
- Dry mouth, changes in sex drive
- Blurred vision, diarrhea
- Weakness, and fatigue
In some cases, severe side effects can include:
- A shuffling walk
- Tremors
- Yellowing of the skin or eyes
- The inability to sit still
- Fever
- Difficulty breathing or swallowing
- Severe skin rash
- An irregular heartbeat, or signs of an allergic reaction (such as a rash, hives, swelling of the face, mouth, hands, lips or tongue, and difficulty breathing)
If any of these effects are experienced, a patient should seek medical assistance immediately.
Benzodiazepine Detox and Withdrawal
Once a person stops using a benzodiazepine, a period of adjustment called withdrawal follows. It can be distressing both physically and psychologically, as the body and brain need time to adjust and recover. During this period, a strong support system of medically trained professionals and recovery support is important. Withdrawal from benzodiazepines can be severe, even dangerous, if a person stops taking the drug too abruptly.
How Long Does Benzodiazepine Withdrawal Last?
The answer to this question depends on the elimination or half-life of the benzodiazepine. Typically, withdrawal begins within one to three days of the last dose, but it can take weeks. There are a number of factors to consider with withdrawal, such as the dosage the person is on, how long they have been taking it, and whether they have been taking a short-acting benzodiazepine. Also, some benzodiazepines can accumulate in the bloodstream after repeated administration, so this may cause prolonged withdrawal symptoms. Initial symptoms include difficulty sleeping, anxiety, and increased heart rate and blood pressure, feeling agitated, and changes in appetite.
The acute phase of withdrawal, known as benzodiazepine withdrawal syndrome, is said to last between five and 28 days. The person usually experiences a peak of severity around one to two weeks post-withdrawal, after which symptoms return to a pre-withdrawal phase. In some cases, the person may experience a protracted withdrawal (also known as post-acute withdrawal syndrome or “PAWS,” for short), which can last for months or longer.
Symptoms of Benzodiazepine Withdrawal
Stopping benzodiazepine medications without professional intervention, such as medical detox, can cause a number of unpleasant and prolonged side effects. Benzodiazepines alter the brain’s chemistry, causing things to slow down. Therefore, abruptly ceasing long-term benzodiazepine use can cause too dramatic a change in brain activity, leading to unpleasant side effects including:
- Nightmares
- Delusions
- Convulsions
- Seizure
- Constipation or diarrhea
- Nausea/vomiting
- Muscle and joint pain
- Migraine headaches
- Intense anxiety
- Irritability
Risks of Home Detox
In this instance, detox is the process of stopping using substance and detoxifying the body at home without medical intervention. Due to the number of health risks associated with home detox, it is not advised by medical professionals. It can be particularly dangerous to suddenly stop drinking or taking drugs cold turkey, rather than tapering off.
Home detox is rarely successful because the side effects of stopping are so unpleasant that the risk of relapse is high.
It is strongly advised by the Substance Abuse and Mental Health Services Administration (SAMHSA) to seek professional intervention, especially if the person has been using substances persistently, to ensure they overcome risks of home detox.
Again, there are a number of risks with home detox—particularly in the cases of alcohol and benzodiazepines. Medically-monitored detox centers are a crucial aspect of the recovery process. They ensure that the person is treated safely and also reduce the risk of complications that might arise from the detox process. According to SAMHSA, almost 80 percent of professional detoxification uses medication to ease withdrawal symptoms.
Benzodiazepine Addiction Treatment
There are various types of benzodiazepine detox, which each depends upon the severity of use.
A medically supervised detox occurs in an inpatient medical detox center or hospital. The benefits of admission are that medically trained professionals are able to closely monitor a person’s progress, administer any medications when necessary, and provide a safe and comfortable environment for the often painful and difficult process of withdrawal.
The Gallus Method of Benzodiazepine Detox
Gallus Medical Detox provides the comfort of a residential facility, but with clinical expertise that is far superior to most detox facilities. We offer safe, effective, and personalized treatment. In fact, we are so proud of our proprietary method that we named it The Gallus Method.
The key features of Gallus Medical Detox include:
- Individual treatment plans, with a focus on personalized sobriety
- Psychological, physical, and social assessments
- IV Therapy Program
- 24/7 medical supervision
- Cardiac telemetry and video technology
- Ongoing adjustments to treatment plans in order to suit our patients’ needs
- An individual aftercare plan identifying resources and next steps toward a long-term recovery
Gallus also offers a unique outpatient benzodiazepine taper support program with medical supervision, MD visits, and individual therapy.
We have addiction treatment centers in Arizona and Colorado, with more opening in coming months.
What our patients say about Gallus Medical Detox
Our patients are the best judge of the quality of our care. Here is what they have to say:
“This place is nothing short of exceptional!”
“I can’t be more pleased, impressed, and grateful with the entire Gallus team.”
“I cannot express in words my deep appreciation for the kindness and very individualized care delivered by motivated and professional caregivers.”
“My stay in this facility was by far the most comfortable I’ve ever experienced. The staff was extremely thoughtful, warm, and informative. Thank you very kindly, everyone.”
Next steps
While detox is usually the first step in recovery, it’s not a cure for addiction. Immediately following detox, behavioral therapy and other addiction treatments should occur while the person is ready to engage in recovery.
You can get more information on detoxing from benzodiazepines here.

 Casey Wilson
Casey Wilson 

 Steve B
Steve B